✭ IVF Technique – A Social Hope

In vitro fertilization (IVF) is one of the most advanced and widely used assisted reproductive technologies (ART) in modern medicine. It has transformed the lives of millions of couples struggling with infertility by providing a scientific method to achieve pregnancy when natural conception becomes difficult or impossible. The term “in vitro” means “in glass,” referring to the laboratory setting in which fertilization occurs outside the human body.
This article provides a detailed, structured, and easy-to-understand explanation of the IVF technique, its stages, importance, benefits, limitations, and its role in modern reproductive science.
In vitro fertilization (IVF) is one of the most advanced and effective fertility treatments available today. It has helped millions of couples around the world who struggle with infertility to achieve pregnancy. IVF is a medical procedure where an egg and sperm are combined outside the human body in a laboratory, and the resulting embryo is then transferred into the uterus.
In simple words, IVF allows fertilization to happen in a controlled environment when natural conception is difficult or impossible.
☆ Introduction to IVF
IVF is a medical procedure in which an egg (ovum) is fertilized by a sperm outside the human body, usually in a controlled laboratory environment. Once fertilization occurs, the resulting embryo is cultured for a few days and then transferred into the uterus of the woman, where it may implant and develop into a pregnancy.
Unlike natural conception, where fertilization occurs in the fallopian tubes, IVF bypasses several biological barriers that may prevent pregnancy, making it a highly effective solution for various infertility conditions.
The term “in vitro” means “in glass,” referring to the laboratory dish used during fertilization. In IVF, the natural process of fertilization is assisted by medical technology.
Normally, fertilization happens inside the fallopian tube. However, in IVF, this step is bypassed, making it a powerful solution for many infertility problems.
☆ Who Needs IVF Treatment ?
IVF is recommended in various medical conditions, including:
- Blocked or damaged fallopian tubes
- Ovulation problems (like PCOS)
- Low sperm count or poor sperm quality
- Endometriosis
- Unexplained infertility
- Age-related fertility decline
- Genetic disorders
IVF gives hope to couples who have tried other treatments without success.
☆ Why IVF is Needed
Infertility can result from multiple causes affecting either the male or female partner, or both. IVF is recommended when other simpler treatments, such as medications or intrauterine insemination (IUI), have failed or are not suitable.
Common conditions where IVF is used include:
- Blocked or damaged fallopian tubes
- Ovulation disorders (e.g., PCOS)
- Low sperm count or poor sperm motility
- Endometriosis
- Unexplained infertility
- Advanced maternal age
- Genetic disorders requiring embryo screening
IVF provides a controlled and precise way to overcome these challenges.
☆ Step-by-Step Process of IVF
The IVF procedure is a multi-stage process that typically takes several weeks to complete. Each stage is carefully monitored by fertility specialists to maximize success rates.
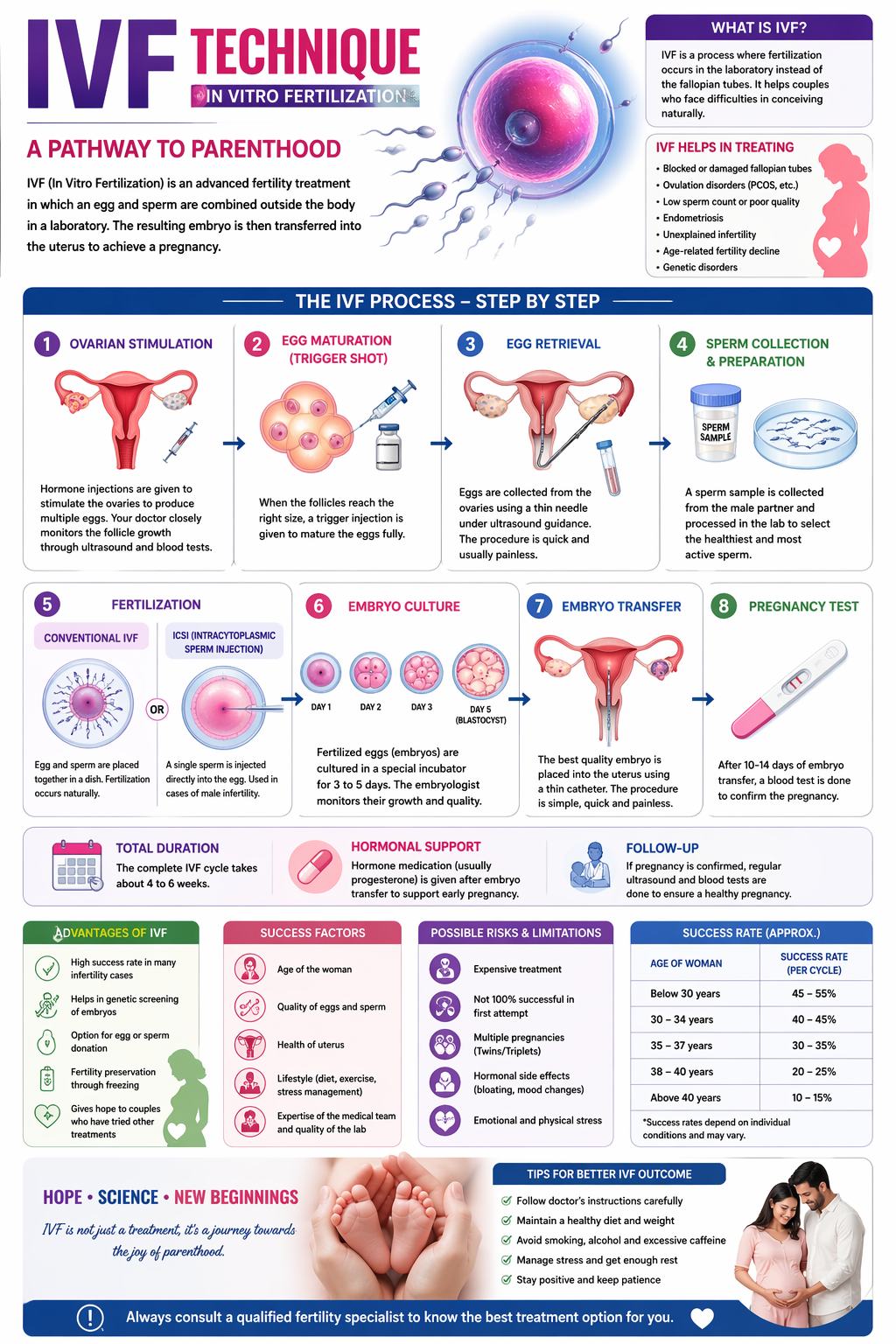
1. Ovarian Stimulation
The IVF process begins with ovarian stimulation. In a natural menstrual cycle, a woman produces one mature egg. However, IVF requires multiple eggs to increase the chances of successful fertilization.
Hormonal medications are administered to stimulate the ovaries to produce multiple mature follicles (fluid-filled sacs containing eggs). These medications usually include:
- Follicle-stimulating hormone (FSH)
- Luteinizing hormone (LH)
- Gonadotropins
During this phase, doctors monitor the patient through blood tests and ultrasound scans to track follicle growth and hormone levels.
The process begins with hormone injections to stimulate the ovaries. Normally, only one egg is released each month, but IVF requires multiple eggs to increase success chances.
Doctors monitor the development of follicles using ultrasound and blood tests.
2. Egg Maturation and Trigger Injection
Once the follicles reach the appropriate size, a “trigger shot” (usually human chorionic gonadotropin or hCG) is given. This injection helps the eggs mature fully and prepares them for retrieval.
Timing is extremely important in this stage. Egg retrieval is scheduled approximately 34–36 hours after the trigger injection to ensure optimal maturity.
When the eggs are ready, a trigger injection is given to help them mature completely. This ensures that the eggs are ready for fertilization.
3. Egg Retrieval (Oocyte Retrieval)
Egg retrieval is a minor surgical procedure performed under sedation or anesthesia. Using ultrasound guidance, a thin needle is inserted through the vaginal wall into the ovaries to collect the eggs from the follicles.
The procedure usually takes 15–30 minutes and is considered safe. After retrieval, the eggs are immediately transferred to the laboratory for further processing.
A minor surgical procedure is performed to collect eggs from the ovaries using a thin needle under ultrasound guidance.
This procedure is quick and usually painless due to sedation.
4. Sperm Collection and Preparation
On the same day as egg retrieval, a sperm sample is collected from the male partner. If necessary, sperm can also be obtained through surgical methods in cases of severe male infertility.
The sperm sample is then processed in the laboratory to select the healthiest and most active sperm cells. This step ensures that only high-quality sperm are used for fertilization.
A sperm sample is collected from the male partner. The healthiest and most active sperm are selected in the lab.
5. Fertilization
Fertilization is the core step of the IVF process. There are two primary methods used:
a) Conventional IVF
Eggs and sperm are placed together in a culture dish, allowing fertilization to occur naturally. Sperm and egg are mixed naturally.
b) Intracytoplasmic Sperm Injection (ICSI)
A single sperm is directly injected into an egg using a fine needle. This method is commonly used in cases of male infertility or previous fertilization failure. A single sperm is injected directly into the egg.
- Fertilization leads to the formation of embryos.
- After fertilization, the eggs are monitored to confirm successful embryo formation.
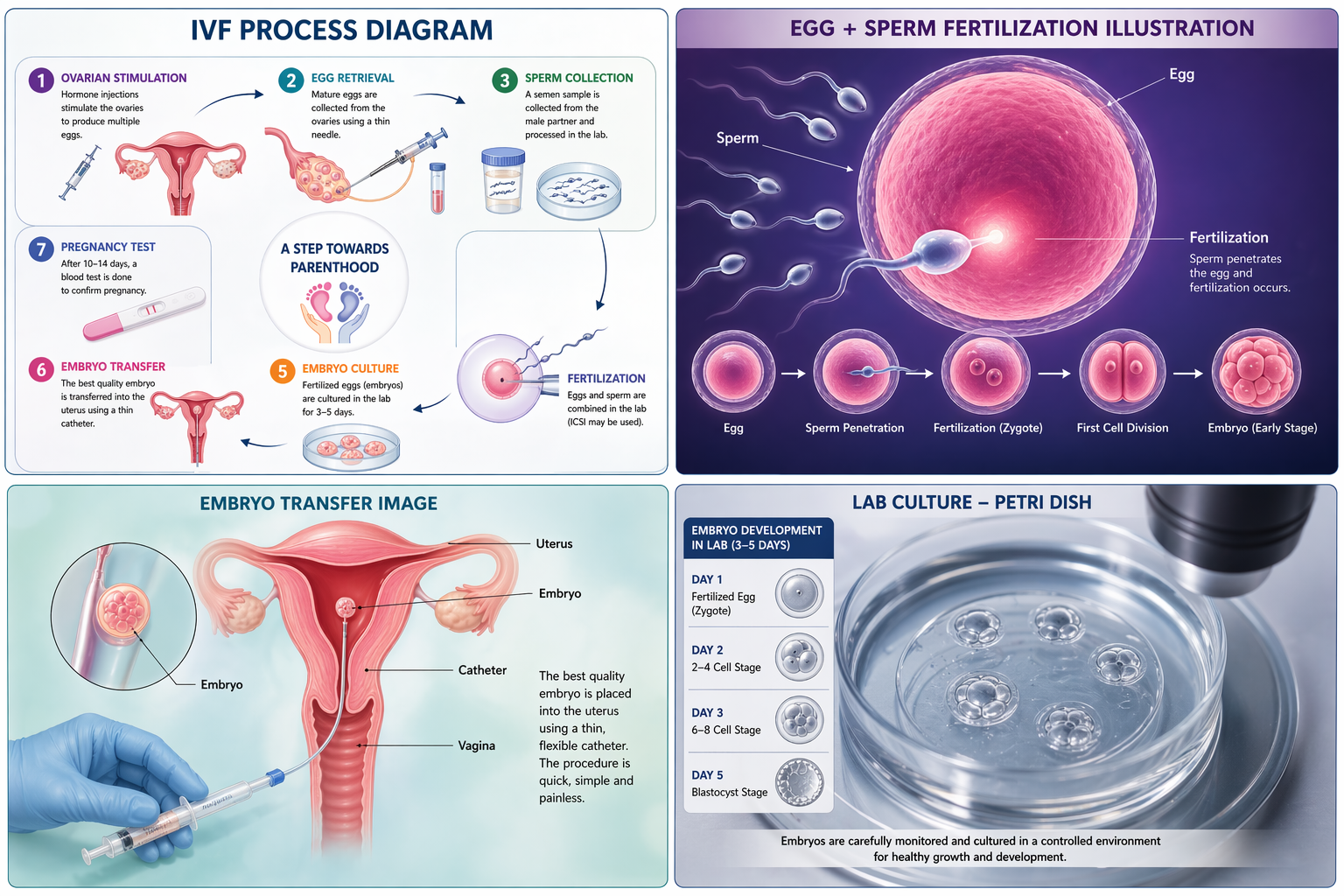
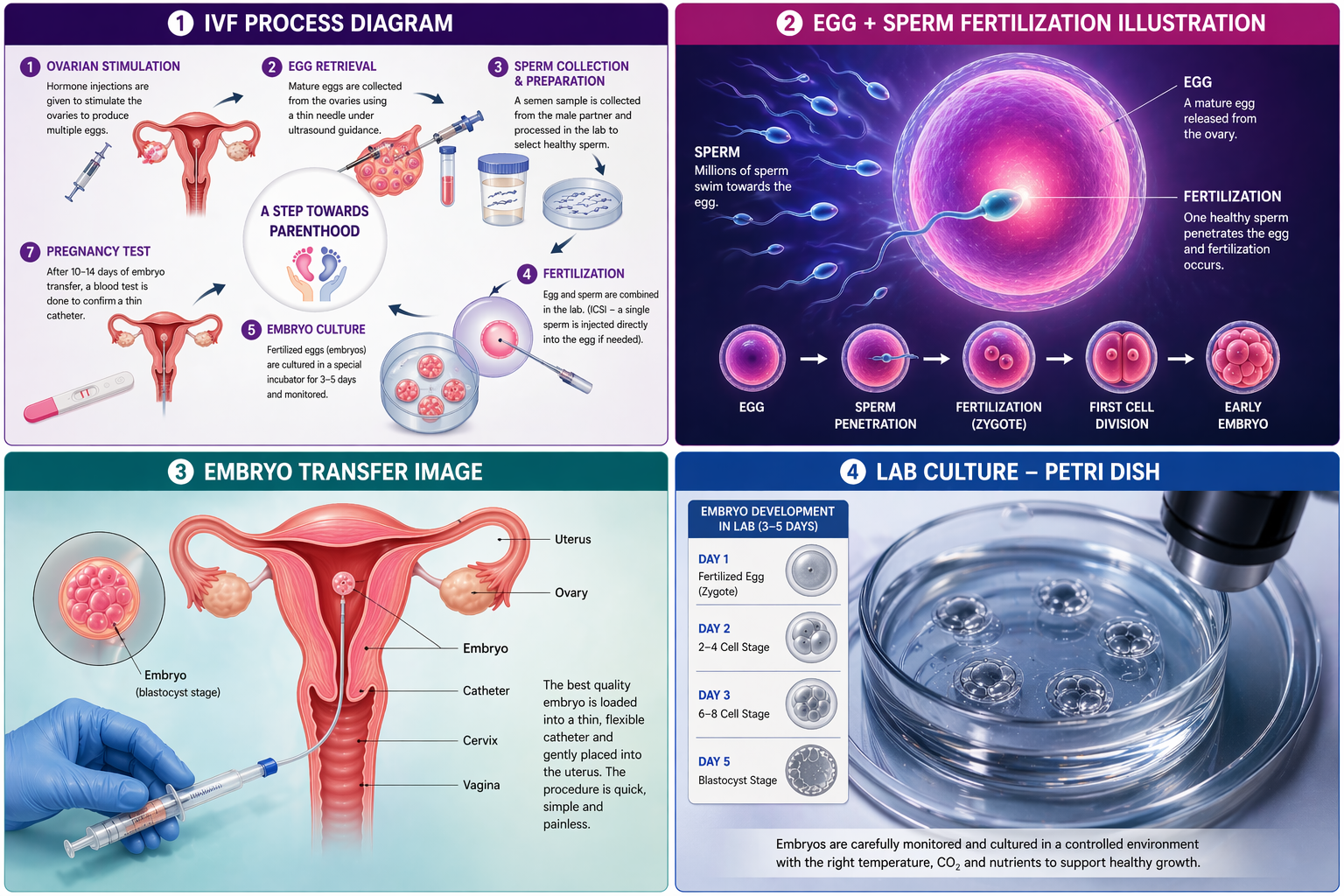
6. Embryo Culture
Once fertilization occurs, the embryos are cultured in a controlled laboratory environment for 3–5 days. During this period, embryologists observe their development and quality.
Embryos go through several stages:
- Cleavage stage (2–4 days)
- Blastocyst stage (5–6 days)
The blastocyst stage is often preferred for transfer because it has a higher chance of implantation.
- The embryos are cultured in the lab for 3–5 days. Doctors monitor their growth and quality.
- The best embryos are selected for transfer.
7. Embryo Selection and Genetic Testing
Not all embryos are equally viable. Specialists select the best-quality embryos based on their appearance and development.
In some cases, genetic testing (Preimplantation Genetic Testing or PGT) is performed to detect chromosomal abnormalities or inherited disorders. This improves the chances of a healthy pregnancy.
8. Embryo Transfer
- Embryo transfer is a simple and painless procedure. A thin catheter is used to place one or more selected embryos into the uterus.
- This step does not require anesthesia and takes only a few minutes. After transfer, the patient is advised to rest briefly.
- A healthy embryo is transferred into the uterus using a thin catheter. This is a simple and painless procedure.
9. Luteal Phase Support
After embryo transfer, hormonal support (usually progesterone) is provided to prepare the uterine lining for implantation and support early pregnancy.
10. Pregnancy Test
About 10–14 days after embryo transfer, a blood test is conducted to check for pregnancy. If successful, further monitoring is done to confirm the development of the embryo. After 10–14 days, a blood test is done to confirm pregnancy.
☆ Advantages of IVF
IVF offers several important benefits:
- Provides a solution for multiple infertility causes
- Allows fertilization outside the body in a controlled environment
- Enables genetic screening of embryos
- Offers options for egg or sperm donation
- Allows preservation of fertility through egg or embryo freezing
- Helps overcome many infertility problems
- Controlled fertilization environment
- Allows genetic screening of embryos
- Option for egg/sperm donation
- Fertility preservation through freezing
It has given hope to couples who otherwise had limited chances of having biological children.
☆ Limitations and Challenges
Despite its advantages, IVF also has certain limitations:
- It is an expensive procedure
- Success rates vary depending on age and health
- Multiple cycles may be required
- Emotional and physical stress can occur
- Risk of multiple pregnancies (twins, triplets)
- Possible side effects from hormone medications
- High cost
- Not always successful in first attempt
- Risk of multiple pregnancies
- Hormonal side effects
Success rates are generally higher in younger women and decrease with age.
☆ Success Rate of IVF
The success of IVF depends on several factors:
- Age of the woman
- Quality of eggs and sperm
- Uterine health
- Lifestyle factors (diet, stress, smoking)
- Health condition
On average, younger women may have a success rate of 40–50% per cycle, while it decreases significantly after the age of 35.
☆ Ethical and Social Considerations
IVF has also raised ethical and social questions, such as:
- Use of donor eggs or sperm
- Embryo selection and genetic testing
- Surrogacy arrangements
- Storage and disposal of unused embryos
Different countries have different laws and guidelines to regulate these practices.
☆ Future of IVF
With rapid advancements in medical science, IVF technology continues to improve. New developments include:
- Artificial intelligence in embryo selection
- Improved genetic screening techniques
- Enhanced cryopreservation (freezing methods)
- Personalized fertility treatments
- Advanced genetic testing
- Improved freezing techniques
These innovations are expected to increase success rates and make IVF more accessible in the future. These innovations are making IVF more effective and accessible.
☆ Conclusion
In vitro fertilization is a revolutionary medical technique that has transformed reproductive healthcare. By enabling fertilization outside the human body, IVF overcomes several biological barriers and offers a reliable solution for infertility.
Although the process involves multiple steps, careful monitoring, and emotional commitment, it provides hope and opportunity for millions of couples worldwide. As technology continues to evolve, IVF is likely to become even more efficient, affordable, and widely available.
For individuals facing fertility challenges, IVF is not just a scientific procedure—it is a pathway to parenthood and a symbol of modern medical progress.
IVF is a revolutionary fertility treatment that has changed the lives of millions of couples. It provides a scientific solution to infertility by enabling fertilization outside the body and increasing the chances of pregnancy. IVF offers hope and opportunity for those struggling to conceive naturally. With continuous advancements in medical science, IVF is becoming safer, more efficient, and more widely available.
☆ You can also search our other Articles :
☆ Click on Following Topics :
IVF Technique – A Social Hope
- 1. Richard Feynman’s Scientific Legacy and Love Story
- 2.
- 3.
- 4.
- 5.


[…] 1. IVF Technique – A Social Hope […]